As a yoga instructor and former professional dancer, I’ve frequently heard people say they wish they were as flexible as I am. But the old adage holds true: the grass isn’t always greener on the other side. During my time as a physical therapist, I’ve learned that the flexibility that earned me praise in gymnastics, dance and yoga may contribute to musculoskeletal injuries, chronic pain, and symptoms of neurological, gastrointestinal, immunological and cardiopulmonary distress.
It probably seems obvious that being very stiff can limit your functioning and contribute to aches and pains. Decreased motion is referred to as hypomobility, and can occur due to a combination of genetics, disuse or aging. But what many people don’t realize is that human mobility exists on a spectrum, and being too far on either side can cause problems.
Opposite of those with limited mobility are people like me, who are hypermobile. While hypermobility can occur locally due to an injury, some of us have genetic influences that make our connective tissue more mobile generally. Excess motion can contribute to injuries like sprains and dislocations, and may require a different approach than “standard” rehabilitation, which tends to be geared toward those who are hypomobile, as hypomobility is more common than hypermobility. Hypermobility is often perceived as benign or even desirable, so it often isn’t a focus of healthcare professionals training. When hypermobile patients aren’t treated with an individualized program that meets their unique needs, they may not respond as expected, and can go on to have persistent issues that potentially worsen over time. It can be very helpful to identify hypermobility and find support for the unique deficits that come with hypermobility, like decreased proprioception (body sense) in order to prevent injury or ensure optimal healing.

Often my first indication that a patient is hypermobile is their choice of sitting position. Rather than sit in a chair in my office like the rest of my patients, they opt to sit on my treatment table in full lotus, “W” sit, or even legs straddled across the width of the table in the splits.
After noticing their choice of sitting postures, I often ask these patients if they have any “party tricks.” They usually light up with a smile and demonstrate their “double-jointedness,” or even their ability to “pop” bones out of place. Hypermobiles often discover these tricks when they are very young as their friends find such maneuvers entertaining. They often gravitate toward activities like dance, gymnastics, or yoga because they can do them easily.

Luckily my PT’s had identified hypermobility at the age of 12 and issued a Pilates program to help help me stay strong throughout my hypermobile range of motion. When my dance career ended, I taught Pilates full-time, which allowed me to learn more about how to create support and stability for hypermobile joints by improving proprioception, motor control, strength and endurance, working first through a smaller, mid-ranges of motion where muscles can best support joint motion and progressing as needed to larger ranges of motion. In PT school, I learned more about how to distribute motion evenly across the kinetic chain to avoid over-stressing any one area, and various manual therapy techniques helped me to improve motion in specific areas that didn’t move as well, which is particularly important as we age and stiffen up (even hypermobiles stiffen with age, and Beighton Scores are known to decrease by the time we reach mid-thirties!)
If your PT suspects that your connective tissue is hypermobile, they may have you perform the following movements to determine your Beighton Score, a general screening tool for hypermobility. Feel free to follow along to self-assess, making sure not to force any excessive motion, moving only through a range that is normal and pain-free for your body:
- Standing with legs straight, bend forward over your legs. If your palms can flatten to the floor, add 1 to your score.

- Stretch both of your knees as far as they can go into extension (often called “locked knees.”) If your knees go beyond 180 degrees, add 1 point for each knee that can hyperextend to at least 10 degrees.
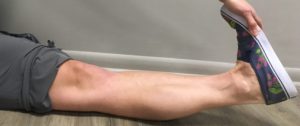
- Straighten your elbows as far as they can go. If they go beyond 180 degrees (often called “double-jointed”) add 1 point for each elbow that hyperextends by at least 10 degrees.

- Bend your thumb toward your forearm. If it touches, add 1 point to your score.
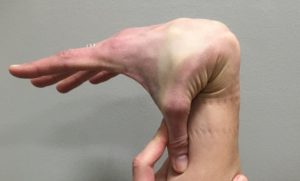
- Bend your pinky backwards. (Update: due to efforts to be more consistent with grading Beighton Scores, it is advised that the hand be flat on a table and all other finger maintain contact with the table, not shown here.) Add 1 point for each pinky that can bend to at least 90 degrees relative to other fingers flat on the table.

If you scored any points, you have localized joint hypermobility. Those with 5 or more points (or 6+ for kids, 4+ for older adults) have generalized joint hypermobility, which was historically called benign joint hypermobility, as hypermobility can occur without any symptoms. The term Hypermobility Spectrum Disorder (HSD) is an updated term that indicates that local or general hypermobility may be symptomatic. Hypermobile Ehlers-Danlos Syndrome (hEDS) is a type of HSD that was first identified by French Drs. Ehlers and Danlos and is thought to be caused by a genetic mutation (although currently this has not been identified.) As such, diagnosis of hEDS is currently based on a mix of objective and subjective conditions, rather than genetic tests that identify other forms of EDS. You can find diagnostic criteria for hEDS here, although I like to remind folks that labels and diagnostic codes are intended to help your medical team to better create an individualized plan that meets your needs, and the difference between HSD and hEDS may not impact treatment. Clinically, HSD and hEDS are treated the same way– by addressing the individual’s complaints and reducing/managing associated risks.
Ideally, all humans will put some effort into maintaining health and wellness. In my experience, those efforts look a bit different for hypermobiles. Muscles that have to do more work to make up for lax ligaments will need to be highly conditioned in order to prevent fatigue, pain and even sensations of “stiffness.” While it might make sense for tighter bodies to stretch when they feel stiff, the sensation of stiffness is a protective mechanism, much like the sensation of pain. Perceived stiffness that is not paired with reduced range of motion doesn’t indicate a need for stretching so much as a need for other kinds of support. Being assessed by a PT who understands hypermobility can be very helpful to establish what specific areas need stretching, and which areas need improved stabilization, strength, blood flow, neurodynamics, sensory integration/proprioception, or recalibration of a sensitized system.
If you are generally hypermobile, exercise is important from a biomechanical perspective as well as neurophysiological one. Although the mechanisms are not entirely clear, hypermobiles tend to have sensitive systems that are prone to neuroimmune dysfunction and heightened pain sensitivity. Appropriate exercise helps to keep these systems running smoothly and downregulate sensitive/sensitized systems, making them less likely to cause chronic symptoms.
While hypermobility is most often considered a musculoskeletal issue, hypermobiles do have increased risk of certain medical conditions that are beyond the scope of this blog, such as gastrointestinal issues, chronic pain and chronic pelvic pain, migraines, chronic fatigue, pelvic organ prolapse, autonomic nervous system dysfunction (dysautonomia/POTS) or heart conditions like valve prolapse or aortic dissection. Therefore, it’s important to find medical professionals who understand the systemic effects of hypermobile connective tissue and can help create a proactive plan to minimize risks and improve symptoms. Finding healthcare professionals (HCP) familiar with these issues may also reduce the harmful effects of being invalidated, misunderstood, or misdiagnosed by HCP’s who simply aren’t aware of these issues and are more likely to ignore/dismiss them or misdiagnose them as more common conditions.
In medicine, there is a saying: “If you hear hoofbeats, think horses, not zebras.” It is intended to remind medical professionals not to overcomplicate things. Hypermobile patients are often the exception to the rule, as we often present with less common issues, and sometimes medically complex conditions. As such, we are frequently referred to as “zebras.” In my own experience, being identified as a zebra was a necessary step in understanding my body’s unique needs, building my support network, and managing my symptoms. Those on the hypermobility spectrum may appear to be healthy, which makes it difficult for others who are unfamiliar with HSD to understand why they struggle with fatigue, pain, “stiffness” or malaise. I hope that sharing my story raises awareness and helps those with hypermobility-related symptoms find the support that they need.
For further information on diagnosis of Hypermobility Spectrum Disorders/Ehlers Danlos Syndromes, you may consider the 2017 EDS International Classification.
Click on these links for more information on Hypermobility Spectrum Disorder and associated symptoms.
I’d love to hear your thoughts about hypermobility! Feel free to share in the comments section below, or contact Dr. Lewan directly.
Kudos. This is a well-done and needed resource. There are a lot of misconceptions out there about EDS and related hypermobility syndromes (not to mention unanswered questions). I see great, reliable, and honest things coming from your blog. If more healthcare providers had this level of comprehension regarding these types of diagnoses then many people would suffer far less. Keep it up!
I can do reverse Namaste, legs up over the back of my neck, fingers folded over each other and I have a dilated left atria. Recently I’ve been diagnosed with POTS. Are all or some of these also EDS qualifiers? Thanks.
Hi Rachel- it does sound like you are on the hypermobility spectrum, but none of the things you mentioned are qualifiers for EDS. Although POTS is highly correlated with EDS, a diagnosis of POTS or dysautonomia is not currently listed as an indication of hypermobile EDS. It is possible that research will clarify the relationship between POTS and EDS and as we learn more, POTS may be added to the diagnostic criteria for hEDS. Nonetheless, it is worth mentioning to your physicians, especially your POTS specialist, that you have some characteristics of hypermobility. Wishing you all the best for health and healing~. C
Here’s a handy list of hEDS diagnostic criteria: https://ehlers-danlos.com/wp-content/uploads/hEDS-Dx-Criteria-checklist-1.pdf
hEDS is the only form that does not have a genetic marker, which is why diagnosis is based on clinical signs. You could see a geneticist to rule out other forms of EDS.
Any thoughts on hypermobility and squatting? My 12 year old daughter is overly flexible and has already has ankle and shoulder problems (popping, partially dislocating, sprains) She always prefers to sit in a squatting position at rest (like with eating, homework time, on the computer). Is this typically a comfortable position for hyper flexible folks and do you think it is safe for her or not a good idea. Thanks!
Deep squatting is generally considered safe as the knee cannot hyper-flex… at some point the calf and the thigh rest against one another allow for passive support that occurs with soft tissue approximation rather than strain to joint/ligaments. Of course, I haven’t seen how she is squatting but I think it is reasonable to assume that this natural physiological movement would be safer than some of the alternatives that hypermobiles develop in order to find more stability, like “W” sitting which may feel good for them because the hip ligaments are strong and they may feel more supported by allowing those ligaments to help support them, even though doing so over time may further increase the laxity of those ligaments. At some point as we grow up, it becomes less socially acceptable for us to use these compensatory strategies (like deep squatting, pretzel sitting, etc.) as an alternative to sitting in the normative posture, so finding a good chair or supportive pillows/devices and conditioning for postural endurance may allow her to be more comfortable for sitting for school, meetings, or work.
At the age of 66 I still w-sit all the time. I can also put my hands flat on the floor when bending over with my legs straight. I am able stretch and reach past my feet, when on the floor. That is further than even my grandkids. Bending over to the side I can go quite far down but can make my hip go out to bend sideways to the floor with my legs straight. I don’t twist my legs around themselves much any more when pretzel sitting.
I never thought this might be related to my constant headaches and migraines. That is interesting.
I am generally fit, as I have been a walker and love many couple and line dances (if we can ever start up again) I am five feet two inches and weigh 125.
Sometimes as I squat down, when I am gardening for example, my femur goes too far sideways (at my knee) and hurts until I straighten my leg, at which time goes back where it belongs. It never is a problem otherwise and doesn’t hurt. Except for my consant headaches (which run in my family) I am hardly ever have pain.
I’m sorry that this is so long. None of my children, I have three, are like this and don’t really have anyone who understands. I do worry that these odd things will one of these days cause me trouble, such as breaking a hip. Is it safe for me to continue to w-sit? The grandkids do get a kick out of my flexibility.
Janice, it sounds like you are a good example of a high functioning hypermobile! It does have perks, especially as we age and our peers become less able to do things like sit on the floor. If you had pain or problems associated with W-sitting, it might make sense to avoid it, but if you’ve been doing it for 60+ years, it sounds like your body has adapted to this activity just fine. It does not increase your risk of fracture– having good mobility may even be protective, as you may simply “bend” rather than “break” if you fell into an awkward position. However, being hypermobile does come with proprioceptive deficits that can increase fall risk, so a balance program to strengthen proprioception and reduce fall risk is advised. As for knee pain with squatting, hip strengthening is an evidence-based approach to improve knee pain that may have additional benefits for your hips– the more mobile a joint is, the more strength we need to best support that joint. Having a lot of hip rotation isn’t a problem in and of itself (some studies would indicate it lessens your risk of osteoarthritis) but having a lot of motion does come with the responsibility of staying strong through that motion and keeping your proprioceptive system healthy so your body can sense/control where you are in space. In short, most folks at your age will need to focus more attention to staying flexible so they don’t lose functional mobility. If you already have a lot of mobility, an individualized program for your body would focus on strength, motor control, and balance/proprioception. All of that can be done with the help of a PT, who should also be able to help with headache pain. In my experience it helps to find a PT that has experience with hypermobility AND spends the better part of an hour with you individually. Some clinic models have PT’s seeing 3 patients at once, in which case everyone gets a more general program (supervised by a rehab aid) that may not meet their individual needs.